Individuals and families who are enrolled in a health plan that is being closed must actively enroll in another plan through Covered California. Those households will not be automatically renewed into a new plan. Without an enrollment selection, the family may have no health insurance at the beginning of 2018. Off-exchange members who have plans being closed will be migrated to a similar plan if the household has not changed their plan for 2018.
California works to combat Trump’s undermining of the ACA
Thanks to the actions of President Trump, in April I took the unprecedented step authorizing health insurers to file two sets of rates for 2018,” said Insurance Commissioner Dave Jones. “We in California are doing everything we can to keep carriers and plans in the individual market, but President Trump continues to undermine the ACA and as these rate filings demonstrate, California is not immune to his efforts to wreck the Affordable Care Act. If President Trump continues down this path, premiums will increase substantially in 2018. The average premium increase doubles if Trump continues to refuse to fund the cost-sharing assistance in the ACA.
Health Net To Drop Walgreens From Pharmacy Network
Members who have used a Walgreens pharmacy at any time in the past 12 months will receive a letter about the change 60 days in advance of the end of the year if they have an individual and family plan. Group members will receive the letter 60 days in advance of their employer’s renewal date. The first letters mail late July to members of groups renewing October 1.
Sutter Reaches Agreement With Health Net For 2017
We are pleased to announce that Sutter Health has come to an agreement with Health Net for 2017. Sutter Health now has agreements in place for 2017 with all major health plans except Blue Shield, with which negotiations continue.
Blue Shield and Health Net Alert Agents to Potential Loss of Sutter Hospitals and Doctors
Blue Shield of California and Health Net are two of the health plans that are currently in negotiations with Sutter Health regarding contracted in-network doctors and hospitals for 2017. Both health insurance companies are alerting agents to the potential that Sutter hospitals and doctors may not be covered in many of their health plans in 2017 if they don’t come to an agreement soon.
Health Net 2017 Californnia Individual and Family Plans
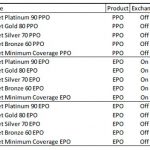
For 2017, Health Net is offering a variety of health plans throughout California. There are EPOs, HSPs, HMOs, and PPOs plans. Some of the plans are offered through Covered California and some, like the PPO plans, are only offered off-exchange direct from Health Net.
Health Net 2016 PPO Plans to be Discontinued
Health Net has announced that they must discontinue their 2016 PPO plans at the request of the California Department of Insurance. Health Net had originally filed for a 23% rate increase for their 2017 PPO plans. Through negotiations with the Department of Insurance, Health Net lowered the rate increase to an average 12.1%. Because of the changes to the PPO plans, Health Net will need to cancel their 2016 PPO Plans on December 31, 2016 and offer a new PPO plan design to new and existing members. On October 4, 2016, the Department of Insurance concluded that the lower rate increase was not unreasonable.
Health Net 2017 Renewal and $50 Gift Card
Health Net of California has announced that all of their 2016 individual and family health plans will roll into 2017. There will be no plan closures making it easier for current members to renew their health plan for the 2017 calendar year. In letters being sent out on September 30, Health Net will be offering a $50 gift card as a reward for certain healthy initiatives on the member’s part.
Health Net requests 23% rate increase for 2017 California individual and family plans
The California Department of Insurance (CDI) has posted the health insurance premium rate increase requests by Health Net for their 2017 California individual and family plans. The overall increase request is 23%, with a maximum for some health plans as high as 34%. The Health Net rate increase would apply to 11,582 members currently in their PPO and EPO health plans.
Health Net requests 15% rate increase for California small group plans
Health Net has filed new small group health insurance premium rates for 2017 with the California Department of Insurance. In the filed rates, Health Net is proposing an average expected annual increase of 15% to their PPO and EPO plans.