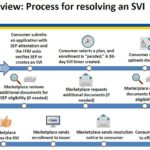
After a consumer has submitted an application under the Special Enrollment Period with a qualifying event, and then selects a health plan, the consumer will have 30 days to verify the qualifying event. The consumer can upload or mail the documentation verifying the qualifying event. The Marketplace will review the documentation and request additional information if necessary.
Notifying Dually-Enrolled Medicare and Healthcare.gov Consumers
Consumers who are identified as enrolled in MEC Medicare and a Marketplace plan through Medicare PDM should return to their Marketplace application and end their Marketplace coverage or Marketplace financial assistance. Consumers may have to pay back all or some of the APTC paid on their behalf for months they had both Marketplace coverage with APTC and MEC Medicare, when they file their federal income tax return.
ACA Proposed Rule Changes for 2018
This rule proposes changes that would help stabilize the individual and small group markets. This proposed rule would amend standards relating to special enrollment periods, guaranteed availability, and the timing of the annual open enrollment period in the individual market for the 2018 plan year; standards related to network adequacy and essential community providers for qualified health plans; and the rules around actuarial value requirements.
Anthem Blue Cross Statement on Trump ACA Executive Order
This Executive Order has no immediate impact on Anthem plans or our members’ benefits and coverage.
Executive Order To Minimize The Economic Burden Of The ACA by President Trump
It is the policy of my Administration to seek the prompt repeal of the Patient Protection and Affordable Care Act (Public Law 111-148), as amended (the “Act”). In the meantime, pending such repeal, it is imperative for the executive branch to ensure that the law is being efficiently implemented, take all actions consistent with law to minimize the unwarranted economic and regulatory burdens of the Act, and prepare to afford the States more flexibility and control to create a more free and open healthcare market.