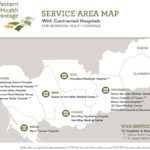
For individuals and families who travel more than 100 miles from their home, WHA plan members will be eligible for assistance with medical consultations and referrals from Assist America at mywha.org/travel. There is also a 24-hour nurse line to answer general health questions and referral to nurses with more specific knowledge of disease management.
Blue Shield Offers Both PPO And HMO Plans In California For 2018
The Blue Shield Trio HMO plans include such medical groups as Dignity Health, Hoag Memorial, John Muir, Providence St. Joseph, St. Jude, and UC San Francisco. Your PCP will refer you to specialists within the network of doctors and providers within his or her medical group. Trio HMO plan will be available in 24 California counties. Trio HMO plan will also include the BlueCard program for urgent care outside of California similar to the PPO plans.
Anthem Blue Cross 2018 California Family Plans
All the plans offered will EPO (Exclusive Provider Organization) with no out-of-network coverage. Anthem will retain the BlueCard for travel coverage for its Blue Cross members. The 2018 plans will continue to use the Pathway network of providers.
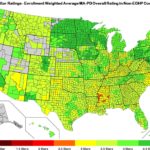
2017 Medicare Advantage Star Ratings By Plan
Medicare Advantage with prescription drug coverage (MA-PD) contracts are rated on up to 44 unique quality and performance measures; MA-only contracts (without prescription drug coverage) are rated on up to 32 measures; and stand-alone PDP contracts are rated on up to 15 measures. Each year, CMS conducts a comprehensive review of the measures that make up the Star Ratings, considering the reliability of the measures, clinical recommendations, feedback received from stakeholders, and data issues.
California works to combat Trump’s undermining of the ACA
Thanks to the actions of President Trump, in April I took the unprecedented step authorizing health insurers to file two sets of rates for 2018,” said Insurance Commissioner Dave Jones. “We in California are doing everything we can to keep carriers and plans in the individual market, but President Trump continues to undermine the ACA and as these rate filings demonstrate, California is not immune to his efforts to wreck the Affordable Care Act. If President Trump continues down this path, premiums will increase substantially in 2018. The average premium increase doubles if Trump continues to refuse to fund the cost-sharing assistance in the ACA.
Covered California Releases 2018 Rates, Plans, And Carriers
Covered California instructed health insurance companies to submit their rates assuming direct payment to fund the CSR subsidies would be continued, but to also submit a separate CSR surcharge to “load” any costs to fund this program onto Silver-tier plans for those who receive subsidies. As a result, Silver-tier consumers may see an additional “CSR surcharge” that averages 12.4 percent — ranging from 8 percent to 27 percent on the gross price of their premiums
Blue Cross Grandfathered Plans 2017 Rate Action
Beginning April 1, 2017, Anthem Blue Cross will adjust the base rates for existing business on all California Department of Insurance (CDI) grandfathered medical plans with an April 1, 2017 effective date. Members will also receive an adjustment for age changes. The base rates for members on Department of Manage Health Care (DMHC) grandfathered medical plans, that were effective April 1, 2016, are not scheduled to change in 2017. DMHC members will receive an adjustment for age changes.
Some Anthem grandfathered members will be receiving a refund
Individual grandfathered members enrolled in Anthem Blue Cross Life & Health Insurance Company (CDI regulated) policies at least one day in September of 2016 will be receiving a refund as a result of funds left over from a 2013 settlement of a class action lawsuit (Kreuzhage v. Anthem). This includes the majority of the grandfathered members. Members on Affordable Care Act (ACA) On and Off Exchange plans, and grandfathered members on Anthem Blue Cross (DMHC regulated) plans are not included.
Covered California Extends Enrollment Deadline to December 17th for January 1, 2017 Start Date
Consumers now have until midnight on Dec. 17 to sign up for health care coverage that will begin on Jan. 1, 2017, Covered California announced.
Blue Shield and Health Net Alert Agents to Potential Loss of Sutter Hospitals and Doctors
Blue Shield of California and Health Net are two of the health plans that are currently in negotiations with Sutter Health regarding contracted in-network doctors and hospitals for 2017. Both health insurance companies are alerting agents to the potential that Sutter hospitals and doctors may not be covered in many of their health plans in 2017 if they don’t come to an agreement soon.