The standard monthly premium for Medicare Part B enrollees will be $134 for 2018, the same amount as in 2017. Some beneficiaries who were held harmless against Part B premium increases in prior years will have a Part B premium increase in 2018, but the premium increase will be offset by the increase in their Social Security benefits next year.
Medicare Special Election Period For Individuals Affected By California Wildfires
Any beneficiary who resides in, or resided in, an area for which the Federal Emergency Management Agency (FEMA) has declared an emergency or major disaster (see www.fema.gov/disasters or the list below*) is eligible for the SEP, if the beneficiary was unable to enroll in a plan during another qualifying election period. In addition, beneficiaries who do not live in the impacted areas but receive assistance from someone living in one of the affected areas also qualify for this SEP.
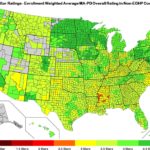
2017 Medicare Advantage Star Ratings By Plan
Medicare Advantage with prescription drug coverage (MA-PD) contracts are rated on up to 44 unique quality and performance measures; MA-only contracts (without prescription drug coverage) are rated on up to 32 measures; and stand-alone PDP contracts are rated on up to 15 measures. Each year, CMS conducts a comprehensive review of the measures that make up the Star Ratings, considering the reliability of the measures, clinical recommendations, feedback received from stakeholders, and data issues.
CMS Reveals New Medicare Card Design
Healthcare providers and people with Medicare will be able to use secure look-up tools that will allow quick access to the new Medicare numbers when needed. There will also be a 21-month transition period where doctors, healthcare providers, and suppliers will be able to use either their current SSN-based Medicare Number or their new, unique Medicare number, to ease the transition.
Confusion Over Medicare and Obamacare Enrollment, CMS Waives Late Enrollment Part B Penalty
CMS is offering equitable relief to certain individuals enrolled in both Medicare Part A and coverage through the Marketplace for individuals and families to enroll in Medicare Part B without penalty. Further, CMS is offering equitable relief to certain individuals who dropped or lost their coverage through the Marketplace and are paying a late enrollment penalty from their subsequent late enrollment into Medicare Part B. These eligible individuals can have their penalty reduced. Individuals can apply for the Medicare Part B enrollment opportunity and reduction in late enrollment penalties during a limited time – it is available now and ends September 30, 2017.
When Is Medicare Primary Or Secondary Payer of Health Care Costs?
Medicare can be the secondary payer in situations where they don’t provide the primary health insurance coverage or when another insurer may have the primary responsibility for covering the claim. However, even when Medicare is the secondary payer, they still may not cover all of the remaining health care costs associated with the claim.
Notifying Dually-Enrolled Medicare and Healthcare.gov Consumers
Consumers who are identified as enrolled in MEC Medicare and a Marketplace plan through Medicare PDM should return to their Marketplace application and end their Marketplace coverage or Marketplace financial assistance. Consumers may have to pay back all or some of the APTC paid on their behalf for months they had both Marketplace coverage with APTC and MEC Medicare, when they file their federal income tax return.
CMS To Phase Out Social Security Numbers On Medicare ID Cards
Providers and beneficiaries will both be able to use secure look up tools that will support quick access to MBIs when they need them. There will also be a 21-month transition period where providers will be able to use either the MBI or the HICN further easing the transition.
UnitedHealthCare Medicare Advantage Plans Fined $2.4 million
CMS identified violations of Part D formulary and benefit administration requirements that resulted in UnitedHealth’s enrollees experiencing inappropriate denials of and/or delayed access to Part D prescription drugs at the point of sale. UnitedHealth’s violations include:
2017 Medicare Parts A & B Premiums and Deductibles Announced
The Centers for Medicare & Medicaid Services (CMS) announced the 2017 premiums for the Medicare inpatient hospital (Part A) and physician and outpatient hospital services (Part B) programs.