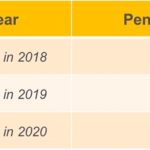
The penalty also remains in effect for 2018 coverage. The only change is the tax penalty will no longer be in effect beginning in 2019.
Trump Watches As Health Insurance Ship Sinks
“This is yet another failing report card for the Exchanges. The American people have fewer insurance choices and in some counties no choice at all. CMS is working with state departments of insurance and issuers to find ways to provide relief and help restore access to healthcare plans, but our actions are by no means a long-term solution to the problems we’re seeing with the Insurance Exchanges,” said CMS Administrator Seema Verma.
Blue Shield Opposes New Trumpcare Plan
the AHCA as currently drafted is flawed as well. The tax credits it provides do not vary based on either a person’s income or the cost of care where they live. There is no help with deductibles and co-pays for those with lower incomes. Millions of people, particularly older Americans, would not be able to afford health insurance or to get care when they need it. In addition, the recent amendments could return us to a time when people who were born with a birth defect or who became sick could not purchase or afford insurance, and when benefits were not there when people needed them the most.
California Authorizes Health Insurers To File “Trump Rates” and “ACA Rates”
Insurance Commissioner Dave Jones announced today that he has authorized health insurers filing rates with the Department of Insurance to file two sets of rates, in light of the market instability created by President Trump’s continued undermining of the Affordable Care Act (ACA).
Covered California Analysis Shows Yuge Price Increases If Trump Plan Implemented
The analysis found that Covered California health plan premiums could rise up to 49 percent if two key elements that have been in place for the past four years are changed: Cost-sharing reduction reimbursements are no longer directly funded as reimbursements to carriers, and the shared individual responsibility payment is not enforced.
California Insurance Commissioner Blasts New Trump ACA Rules
The misnamed “market stabilization” rules sabotage the Affordable Care Act by significantly reducing the open enrollment time period and creating other conflicts with state laws. Like President Trump’s threats to eliminate the cost-sharing subsidies, his new regulations will destabilize, rather than strengthen, the health insurance market.
IRS Loosens ACA Individual Mandate Health Insurance Reporting For 2016
The IRS announced to tax preparation professionals that they will not reject a tax returns because the tax payer has not indicated whether they had health insurance coverage for 2016. Under the ACA, if a tax payer has not had health insurance for most of 2016, they are subject to the Shared Responsibility Payment also referred to as the Individual Mandate.
Anthem Blue Cross Statement on Trump ACA Executive Order
This Executive Order has no immediate impact on Anthem plans or our members’ benefits and coverage.
Executive Order To Minimize The Economic Burden Of The ACA by President Trump
It is the policy of my Administration to seek the prompt repeal of the Patient Protection and Affordable Care Act (Public Law 111-148), as amended (the “Act”). In the meantime, pending such repeal, it is imperative for the executive branch to ensure that the law is being efficiently implemented, take all actions consistent with law to minimize the unwarranted economic and regulatory burdens of the Act, and prepare to afford the States more flexibility and control to create a more free and open healthcare market.
Anthem Analysis of Trump and Republican Positions on Obamacare
We conducted an analysis of the House Republican Platform released over the summer, which may serve as a starting point for legislative changes. The below chart shows how some of President-elect Trump’s campaign proposals line up with the House Republican Platform released earlier this year.