The Department of Health Care Services notified all county welfare directors in a letter dated July 31, 2017, that for eligibility determinations, same-sex married couples will be treated the same as opposite-sex married spouses. One of the significant changes is that county eligibility workers will no longer have to request verification of the same-sex marriage. They same-sex couple, regardless of which state they were married in, will just have to attest under penalty of perjury that they are legally married.
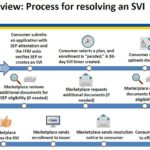
Healthcare.gov Special Enrollment Verification Phase II: Marriage, Adoption, Medicaid
After a consumer has submitted an application under the Special Enrollment Period with a qualifying event, and then selects a health plan, the consumer will have 30 days to verify the qualifying event. The consumer can upload or mail the documentation verifying the qualifying event. The Marketplace will review the documentation and request additional information if necessary.